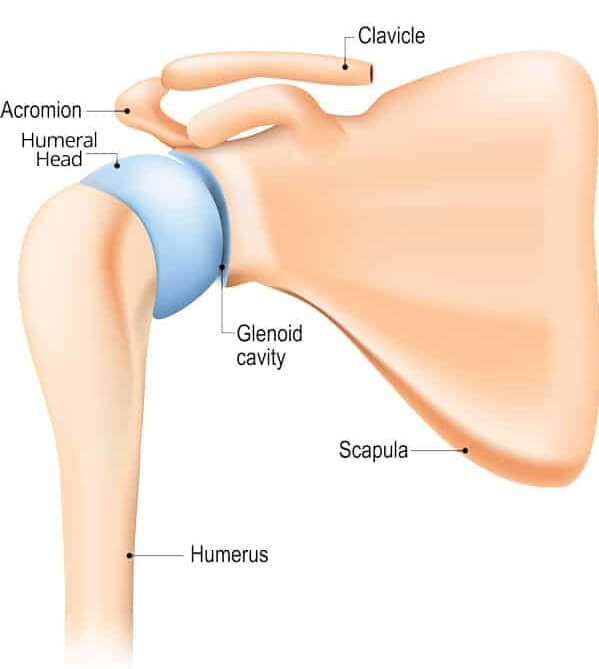
 The shoulder joint, also known as the Glenohumeral joint, is a ball & socket articulation of the humeral head (ball) of the upper arm bone and the glenoid cavity (socket) of the shoulder blade.
The shoulder joint, also known as the Glenohumeral joint, is a ball & socket articulation of the humeral head (ball) of the upper arm bone and the glenoid cavity (socket) of the shoulder blade.
The shoulder joint is one of the largest and most complex joints in the body allowing it to move in almost any direction. This allows the arm to rotate in a circular fashion—such as throwing a baseball—and to hinge out, up, and away from the body—as in the motions associated with performing jumping jacks.
The many different components of the shoulder work in unison to keep it positioned properly. Damage to these components can cause instability within the joint leading to limited range of motion and a significant amount of pain.
What is Shoulder Instability?
Shoulder instability occurs when key components of the surrounding structure of the shoulder joint become stretched, torn, or detached allowing the humeral head to slip out of its place within the glenoid socket.
Types of Shoulder Instability
Shoulder instability can be categorized into two main types:
- Traumatic shoulder instability is caused by injury or trauma—such as a fall on an outstretched hand or forceful blow to the shoulder—which damages the supporting structure of the joint. Traumatic shoulder instability is most common among athletes due to an increased risk of recurrent injury.
- Atraumatic shoulder instability occurs when a patient has a general laxity or looseness in their ligaments allowing the shoulder to shift in and out of the socket. This can be due to a congenital condition or can occur over time.
Those born with hypermobility or generalized looseness within the shoulder are typically able to rotate their arms beyond the normal range of motion. This increased motion can cause frequent sprains, subluxations, or dislocations of the joint.
Atraumatic instability is most commonly caused by repetitive overhead motion. This is often seen among athletes and patients who hold jobs requiring routine overhead activities. Over time, this repetitive motion can damage the tissue and ligaments surrounding the joint.
Shoulder Dislocation and Subluxation
A shoulder dislocation occurs when the humeral head (ball) completely separates from the shoulder socket. Shoulder subluxation is a partial dislocation where the shoulder shifts out of place, but not completely out of the socket. Both shoulder subluxation and shoulder dislocations share common symptoms—although, the severity of dislocation is usually much greater.
Symptoms of a dislocated shoulder joint may include:

- A “popping” sensation at the time of dislocation
- Severe pain in the shoulder or upper arm
- Visible deformity such as a bump on the front of the shoulder or in the armpit
- Numbness or tingling along the arm
- Weakness in the arm
- Severely restricted range of motion
- Affected shoulder may appear to hang down and forward creating a large dimple just below the shoulder blade near the collarbone
- Muscle spasms may occur in the shoulder
A young, active patient who has suffered from a subluxation or dislocation is likely to experience repeat dislocations leading to chronic instability. The risk for recurrence can be as high as 60% with each dislocation causing more wear and damage to the shoulder. Older patients are typically less likely to experience recurrences due to the body naturally stiffening as we grow older. Older patients who have weakness after a shoulder dislocation should be ruled out for rotator cuff tear as these injuries can be common.
Although the shoulder can be displaced in multiple directions, anterior (front) dislocations are the most common making up for more than 95% of reported cases. wiki
Bankart Lesion
When the humeral head is dislocated, it can often cause damage to the connective tissue around the rim of the glenoid “socket”, called the labrum. This is known as a Bankart lesion, or labral tear. A Bankart tear can occur at the front or back of the shoulder and can cause the joint to dislocate more easily over time.
In some cases, a small piece of the glenoid bone can be torn off with the labrum. This is known as a bony Bankart lesion and may require surgical intervention to repair damage.
Treatment Options for Shoulder Instability
Diagnosis typically includes a physical exam and x-rays to determine the exact cause of instability. If needed, advanced imaging techniques, such as an MRI, may be used to determine the extent of damage.
Both surgical and non-surgical treatment options are available and should be determined based on factors such as:
- Cause and extent of instability
- Age and activity level of the patient
- Associated injuries or dislocations (past or present)
- Damage to the bone, cartilage, and surrounding tissue
In some cases, non-surgical treatment may be successful in reducing symptoms. However, when damage is severe or risk of recurrent dislocation interferes with normal use of the shoulder, surgical intervention may be recommended.
Non-surgical treatment for shoulder instability may include:
- A sling or shoulder brace to immobilize the shoulder
- NSAIDs such as aspirin or ibuprofen to reduce swelling and pain
- Physical therapy to improve range-of-motion and strengthen the surrounding muscles
- Ice packs applied to the shoulder before and after exercise or activity to reduce swelling
Surgical treatment for shoulder instability may include:
- Bankart Repair: Also known as labral repair, this procedure is used to repair tears to the labrum. Labral repair is typically performed arthroscopically on an outpatient basis.
- Latarjet Technique: Damaged bone in the front of the glenoid socket is a common cause of frequent dislocation. When this occurs, the Latarjet procedure is used to transfer bone and muscle from another part of the shoulder to keep the humeral head (ball) in place.
- Remplissage Technique: This procedure is used to “fill” a dent in the humeral head, known as a Hill-Sachs lesion. This is achieved by advancing part of the attachment of the rotator cuff, filling the dented area. The Remplissage technique is most commonly performed in conjunction with Bankart repair.
- Capsular Shift: This procedure is used to tighten the joint capsule containing the ligaments that help to stabilize the shoulder. This is done by “tucking” and suturing the capsule to reduce looseness. A capsular shift is most commonly used in cases of multidirectional instability.
How can we help?
Too often, patients are left unaware of options involving specialty surgeries outside of the surgeon’s “comfort-zone”. Our specialized surgeons are fellowship trained in a variety of surgical procedures, including minimally invasive/arthroscopic treatment, open reconstruction, and procedures involving bone loss. Our expertise allows us to provide our patients with a comprehensive, step-by-step pathway to improving shoulder function.
While we focus on preserving the joint whenever possible using minimally-invasive methods, some patients can require a shoulder replacement to relieve their pain and improve their function. When needed, our fellowship-trained shoulder replacement specialists are available for consultation and will guide you through the process.