 Fractures can occur in many ways, to people of all ages. No matter the cause, the experience is not one easily forgotten. Unfortunately for many, the memory is not the only thing that lingers.
Fractures can occur in many ways, to people of all ages. No matter the cause, the experience is not one easily forgotten. Unfortunately for many, the memory is not the only thing that lingers.
Traditionally, treatment plans for ankle fractures focus only on returning the bones to their normal position and allowing them to heal. While the fracture itself may heal successfully, associated cartilage damage often goes unrecognized leading to persistent pain and, potentially, the development of arthritis.
Fortunately, minimally invasive procedures are now available which allow us to discover and address damaged cartilage in earlier phases of treatment.
What is an Ankle Fracture?
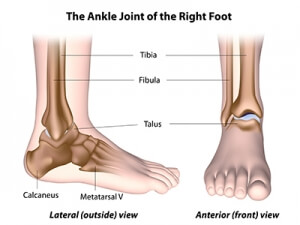
The ankle is made up of three bones–the tibia (shinbone) and fibula of your lower leg and the talus, which sits between the bones of the lower leg and the heel.
An ankle fracture is a break in one or more of the bones making up the ankle joint, typically the tibia or fibula. Fractures are most commonly the result of a high energy impact, such as a sports injury, car accident, or a fall from high elevation. However, when bones are weakened by osteoporosis or other physical conditions, fractures can occur with much lower impact.
Ankle Fracture Types and Treatment
Appropriate treatment for a broken ankle depends on the type and severity of the injury. Ankle fractures can range from a single break in one bone to multiple breaks which can cause displacement, or shifting, of the bones from their normal positioning.
If the position of the bone is intact and the ankle is stable, simple breaks can often be treated without surgery, however, when the bone is displaced, surgery is usually required to realign the bones and reestablish stability.
Symptoms of an Ankle Fracture
It can be easy to mistake an injury to the ankle as a sprain or a soft tissue injury, so it is important to pay attention to these signs and symptoms which may indicate a broken bone:
- An immediate acute, throbbing pain
- Sensitive to the touch, tender
- Unable to put weight on the injured ankle, weight bearing
- Limited, or no movement of the ankle joint
- Immediate swelling and bruising
- Deformed or protruding bones
If you experience any of these symptoms after an injury, it is best to see your doctor or physician to identify the extent of the injury and determine the best course of treatment.
How Can an Ankle Fracture Cause Long-Term Joint Damage?
 The ends of the bones within the ankle joint are covered by articular cartilage, a type of smooth tissue that allows the bones to glide over each other with very little friction. When the stability of the ankle is disrupted, abnormal contact between the bones can wear down the cartilage surrounding them.
The ends of the bones within the ankle joint are covered by articular cartilage, a type of smooth tissue that allows the bones to glide over each other with very little friction. When the stability of the ankle is disrupted, abnormal contact between the bones can wear down the cartilage surrounding them.
When the cartilage is damaged, friction and compression within the joint can cause pain, immobility, and, without treatment, can lead to early onset arthritis.
Cartilage damage is one of the most common causes of persistent pain following an ankle fracture. If you experience pain or weakness beyond the original rehabilitation period, be sure to visit your doctor to determine the cause. Click here to learn the symptoms of cartilage damage.
Ankle Arthroscopy
Although it is not considered a standard procedure in ankle fracture treatment, the use of ankle arthroscopy continues to gain popularity in cases showing increased risk of cartilage damage.
Potential risk factors include:
- Unique fracture pattern
- Dislocation or high level of instability
- Significant bone displacement
- Multiple fracture lines
Ankle arthroscopy is performed using a tiny camera (arthroscope) and surgical tools which are inserted through small incisions in the ankle. Through these incisions, we can view and repair injuries within the deeper layers of the joint with minimal disturbance to the surrounding tissue. By combining arthroscopic techniques with traditional fracture treatment techniques, we are able to treat the injury in its entirety, in an attempt to prevent long-term damage to the joint.
If you have questions or would like to schedule a consultation, please contact our office today.