 Articular cartilage is a type of smooth gliding material that covers the ends of bones within the joints allowing them to glide smoothly with motion. Cartilage lacks the blood supply found in other types of tissue and, therefore, has limited ability to heal on its own. This makes cartilage preservation essential to overall joint health.
Articular cartilage is a type of smooth gliding material that covers the ends of bones within the joints allowing them to glide smoothly with motion. Cartilage lacks the blood supply found in other types of tissue and, therefore, has limited ability to heal on its own. This makes cartilage preservation essential to overall joint health.
In comparison to cartilage found in the larger joints—such as the hip, knee, and shoulder—cartilage in the ankle is quite thin. Since the ankle often bears the weight of the entire body, the small surface area of ankle cartilage leaves it particularly susceptible to damage.
When the cartilage is damaged, friction and compression within the joint can cause pain, immobility, and, without treatment, can lead to early onset arthritis.
Common Causes of Ankle Cartilage Damage
The most common causes of cartilage defects are acute or chronic injuries such ankle sprains, dislocations, fractures, or instability.
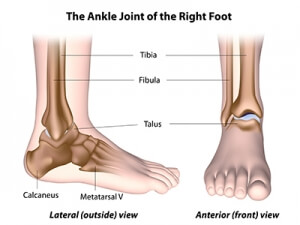
The ankle joint is formed by the tibia, the fibula, and the talus—which is located above the heel bone and helps to transfer pressure evenly across the ankle. When the structure of the ankle is compromised, abnormal contact can occur between the talus and the tibia and/or fibula causing damage to the cartilage. In some cases, the underlying bone is also damaged—this is called a “talar dome lesion” or an osteochondral lesion.
Following a cartilage injury, the body will attempt to repair the damage with a scar-type tissue called fibrocartilage; however, the cartilage is often unable to completely heal on its own. As a result, symptoms may worsen increasing the risk of further damage and the development of arthritis.
Fortunately, with early intervention, we are able to accelerate the healing process and prevent irreparable joint damage.
Symptoms of Cartilage Damage
 Following an ankle injury, symptoms may resolve with treatment; however, if the cartilage is damaged, symptoms often return with activity.
Following an ankle injury, symptoms may resolve with treatment; however, if the cartilage is damaged, symptoms often return with activity.
Symptoms may include:
- Dull or aching pain deep within the joint
- Inflammation
- Stiffness
- Weakness
- Limited mobility
- Locking or catching feeling
Treatment & Recovery
Diagnosis
When a cartilage defect is suspected, a weight-bearing (standing) X-ray is ordered to view the ankle bone anatomy. An x-ray will show if there is substantial arthritis or damage that goes deep into the bone; however, some less obvious or apparent cases may require an MRI for a more detailed view of the joint to determine if there are any osteochondral defects present.
MRIs are most commonly indicated among younger patients or athletes with persistent pain or swelling in the joint that has not responded to the RICE method (rest, ice, compression, and elevation).
Treatment
Treatment options vary depending on the extent and placement of the damage as well as patient factors such as age, weight, and health. Initial treatment typically involves a period of non-weight bearing or protective weight-bearing activity to allow the cartilage to heal. Intra-articular injections may be considered as a short-term option to reduce inflammation, ease pain, and promote healing.
When conservative treatment is unsuccessful or the lesion has progressed beyond the point of healing, surgical intervention may be necessary to repair the damaged cartilage.
Surgical Techniques
Ankle Arthroscopy
Many procedures used in cartilage restoration are performed arthroscopically. A tiny camera (arthroscope) is inserted into the joint through small, minimally invasive incisions allowing specialists to visualize the entire cartilage layer and identify any full thickness defects or loss of cartilage.
Microfracture Surgery
Most commonly performed among younger patients with single, smaller lesions, the microfracture technique is used to promote cartilage development and, thus, facilitate healing.
Through arthroscopic surgery, fragments and debris are cleaned out and loose or damaged sections of bone and tissue are removed to create a stable border. Tiny holes are then drilled into the bone’s surface releasing a combination of blood and bone marrow which form a “super clot” that covers the bone and stimulates the development of fibrocartilage.
Cartilage Transplantation
If a lesion is too large for successful microfracture treatment, a graft can be taken from the patient’s knee, or a cadaver and placed within the cartilage defect to recreate the damaged area. Transplantation is typically done through an open procedure and requires a longer rehabilitation period; however, in more serious cases, it is a viable option for repairing damage and preventing the need for more invasive procedures, such as ankle replacement or ankle fusion.
Recovery
Following treatment, patients will go through a period of non-weight bearing activity to allow the cartilage to heal. On average, this period lasts approximately 4-6 weeks, however, your doctor will discuss a timeline with you based on the extent of your injury and your personal needs. When your doctor has determined sufficient healing, weight-bearing activity will be initiated progressively to get you back to activity in a timely manner. A physical therapy and rehabilitation program will follow to restore range of motion and strength to the ankle.
At Towson Orthopaedic Associates, we work closely with each patient to determine the best possible treatment plan. Our fellowship trained foot and ankle surgeons, Dr. Jeffrey Brodie and Dr. Kenneth DeFontes, offer a variety of minimally invasive options for ankle treatment with a focus on preserving the long-term health of the joint and preventing the development—or progression—of arthritis.
We, at the Joint Preservation Center, understand all patients have different needs and deserve specialized treatment. Contact us today to discover which treatment options are right for you.
 The Joint Preservation Center at Towson Orthopaedic Associates offers an innovative, personalized approach to long-term joint health. Utilizing early diagnosis, intervention, and the latest techniques, our orthopaedic surgeons can restore and preserve the joint’s natural ability, which makes it possible to avoid more invasive surgeries and prolonged rehabilitation. Are you suffering from persistent joint pain or stiffness? Call 410-337-7900 to schedule an evaluation or click here to learn how we can help preserve or restore the health of your joints.
The Joint Preservation Center at Towson Orthopaedic Associates offers an innovative, personalized approach to long-term joint health. Utilizing early diagnosis, intervention, and the latest techniques, our orthopaedic surgeons can restore and preserve the joint’s natural ability, which makes it possible to avoid more invasive surgeries and prolonged rehabilitation. Are you suffering from persistent joint pain or stiffness? Call 410-337-7900 to schedule an evaluation or click here to learn how we can help preserve or restore the health of your joints.